EYESIS low pulse energy has superior effect on children with chalazion
Chalazion (also called meibomian gland cyst) is a common eye disease in children. Its pathogenesis is mainly related to excessive secretion of meibomian glands in children. The retention of gland secretions causes blockage of the outlet of the meibomian gland, which forms chronic inflammatory granuloma of the meibomian gland. In addition, bad habits such as eating fried food and spicy food, as well as causes such as blepharitis, MGD, vitamin A deficiency, and congenital structural abnormalities will also increase the risk of chalazion.

Although the effect of surgery and hormone therapy on children's chalazion is significant, children generally have problems such as poor compliance and high hormone sensitivity. In addition, parents are more inclined to conservative treatment such as hot compress, microwave, antibiotic eye drops, etc., so it is particularly important to choose a conservative treatment suitable for children. In March 2022, Wang Jiancang's team from Hebei Children's Hospital published a clinical study in the Chinese Journal of Strabismus and Pediatric Ophthalmology, which showed that the effect of intense pulsed light on children's chalazion was better than traditional hot compress therapy, and it could be used as a physical therapy option for children's chalazion.



Group data
58 children with chalazion from June 2021 to December 2021 were selected. There were 31 males and 27 females, who were randomly divided into hot compress group and intense pulse group.
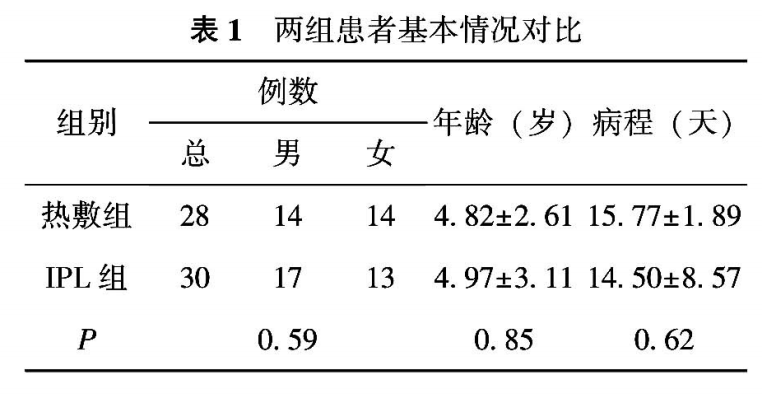
There were 28 patients in the hot compress group, including 14 males and 14 females, with an average age of 4.82 ± 2.61 years and an average course of disease of 15.77 ± 1.89 days;
There were 30 patients in the intense pulsed light group, including 17 males and 13 females, with an average age of 4.97 ± 3.11 years and an average course of 14.50 ± 8.57 days. There was no significant difference between the two groups (P>0.05).
Methods
1、 The hot compress group was treated with hot compress and local application of antibiotics (gatifloxacin eye gel, 1 drop each time, 3 times a day). Take the patient in supine position, soak the patient in warm boiled water with medical gauze, wring out the water and put it to warm, wrap it outside the thermos bottle (at a temperature of about 40 ℃), apply it to the eyelid, and instruct the patient to lie still with eyes closed, once a day for about 15 minutes;
2、 The intense pulsed light (IPL) group was treated with MDC EYESIS light pulse therapeutic apparatus combined with local antibiotics (gatifloxacin eye gel, 1 drop each time, 3 times a day). The output power of EYESIS light pulse therapeutic instrument is 8-12J/cm2, which is completed by the same ophthalmologist.
Effct Standards
(1) Cure: the cyst disappears, and the child has no conscious symptoms;
(2) Effective: the cyst was significantly reduced after treatment compared with that before treatment;
(3) Ineffective: the cyst has no obvious change or obviously increases after treatment.
Total effective rate=(number of cured cases+number of effective cases)/total number of cases × 100%。
Effect Compare
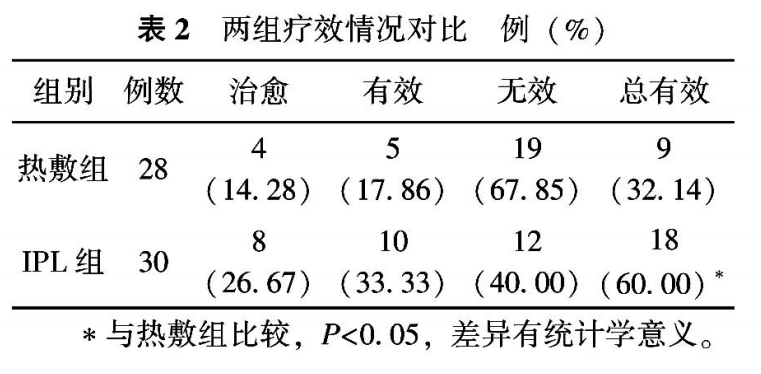
The curative effect of the two groups was compared. The cure rate of IPL group was 26.67% higher than that of hot compress group (14.28%), with no significant difference (P>0.05). However, the total effective rate of IPL group was 60.00% higher than that of hot compress group 32.14%. The difference was statistically significant (P<0.05).
Cases Analysis
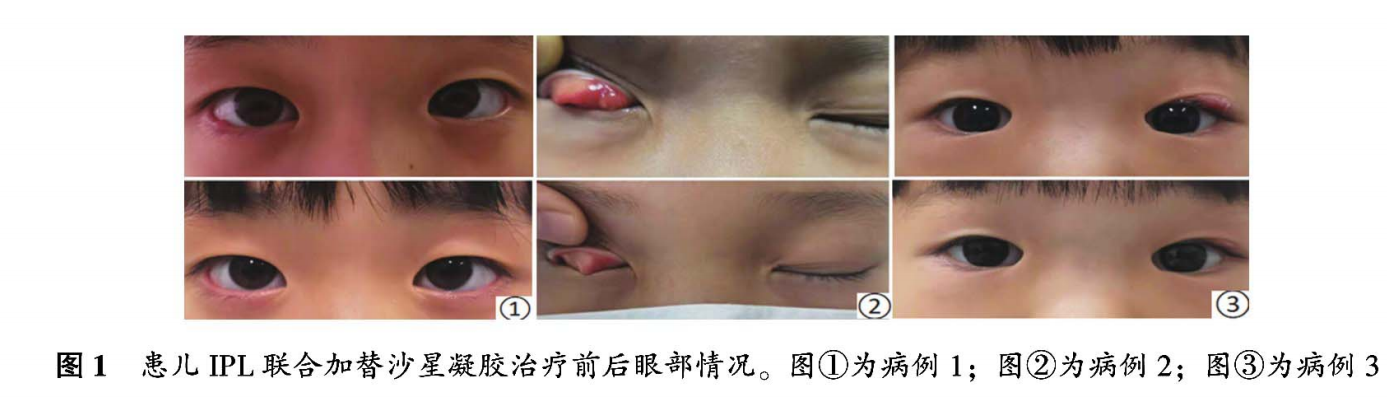
Case 1: Child, 6 years old. The main cause was the right eyelid tumor found for 15 days. 20 days before surgery, bilateral meibomian gland cyst was removed. Physical examination: A induration can be seen on the lower eyelid of the right eye, with local redness and swelling, slight congestion of the eyelid conjunctiva, no congestion of the bulbar conjunctiva, and clear cornea. Left outer eye (1). IPL combined with gatifloxacin eye drops gel treatment, 3 weeks after the tumor disappeared, no recurrence. See ① in Figure 1 below.
Case 2: The patient was a 7-year-old male, who had been hospitalized for 10 days due to the discovery of a right eyelid tumor. Physical examination: A tough mass can be found on the nasal side of the upper eyelid of the right eye, granulation tissue can be seen on the corresponding surface of the eyelid conjunctiva, the eyelid conjunctiva is congested, the bulbar conjunctiva is not congested, and the cornea is clear. Left outer eye (1). After IPL combined with gatifloxacin eye drops with gel, the tumor basically disappeared after 3 weeks. See ② in Figure 1 below.
Case 3: The affected child was 4 years old, and the main reason was that the left eyelid tumor was found for 26 days. Physical examination: local skin on the temporal side of the upper eyelid of the left eye was raised, the surface skin was red and swollen, the tumor corresponded to conjunctival congestion, there was no obvious congestion in the bulbar conjunctiva, and the cornea was clear. Right outer eye (1). After 3 weeks of IPL combined with gatifloxacin eye drops with gel, the tumor was significantly reduced. See ③ in Figure 1 below.

As a new type of dry eye physiotherapy, EYESIS intense pulsed light has been proved by many studies to have multiple effects such as eliminating inflammation, liquefying eyelid fat, dredging tarsal gland, and eliminating demodex. It is speculated that the therapeutic effect of EYESIS on children's chalazion is derived from the comprehensive action mechanism of the above multiple effects.
In addition, the clinical application characteristics of intense pulsed light are also worthy of attention. Compared with surgical treatment and hormone therapy, intense pulsed light is non-invasive, safe, and can improve the function of meibomian gland while treating chalazion in children. Compared with the traditional hot compress, the intense pulsed light has the characteristics of simple and fast operation. Therefore, intense pulsed light can be considered as one of the physical therapies to treat children's chalazion, so as to provide more options for parents to eliminate their concerns.

