Clinical application of IPL in treating ocular surface diseases
Intense pulsed light (IPL) is a kind of high intensity, pulsed and wide spectrum light, covering a wavelength range of 500~1200 nm (visible light and near-infrared light). Its main mechanism of action is based on selective photothermolysis, that is, controlling emission through filters can effectively affect target cell tissues without damaging the pulse light spectrum of other cell tissues.
The principle of selective photothermal interaction was first proposed by Dr. Rox Anderson and published in the authoritative journal Science in 1983. In 1994, intense pulsed light began to be commercially used as a medical technology, and was widely used in dermatology and medical cosmetology. In 2002, when Dr. Rolando Toyos used intense pulsed light to treat rosacea and rosacea, he found that intense pulsed light can increase the local temperature of the subcutaneous meibomian gland, which has a therapeutic effect on meibomian gland dysfunction (MGD).


With the gradual promotion and in-depth study of the clinical application of intense pulsed light in ophthalmology, people found that the mechanism of intense pulsed light mainly includes four functions: anti-inflammatory, heating, antibacterial, and light regulation. The review paper published by Dong Wenhui and Yan Xiaoming from Peking University First Hospital in 2020 explained in detail the mechanism of intense pulsed light in treating ocular surface diseases:

1、 Improves eye tissue - inhibits vasodilation
Reduce the vascularization of the palpebral margin and inflammatory mediators. When IPL irradiates abnormal blood vessels, hemoglobin absorbs light with a wavelength of 580nm or so and converts it into heat, leading to abnormal blood vessel contraction and occlusion and reducing the release of inflammatory mediators.
Restore the meibomian gland hypoxia environment. The meibomian gland is a low oxygen consuming tissue. IPL treatment can restore the hypoxia environment of the meibomian gland by closing abnormal dilated blood vessels, promote the epithelial differentiation of meibomian gland cells and stimulate their secretion function.
2、 Heating of eyelid fat - liquefaction of eyelid fat secretion
The melting point of normal eyelid fat is 28 ℃, while that of MGD patients can reach above 32 ℃. IPL can make the temperature of eyelid fat reach 34 ℃, so as to liquefy the eyelid fat and make it discharge smoothly from the glandular duct, and then achieve the effect of improving the obstruction of meibomian gland. The treatment effect can be improved by combining with meibomian gland massage.
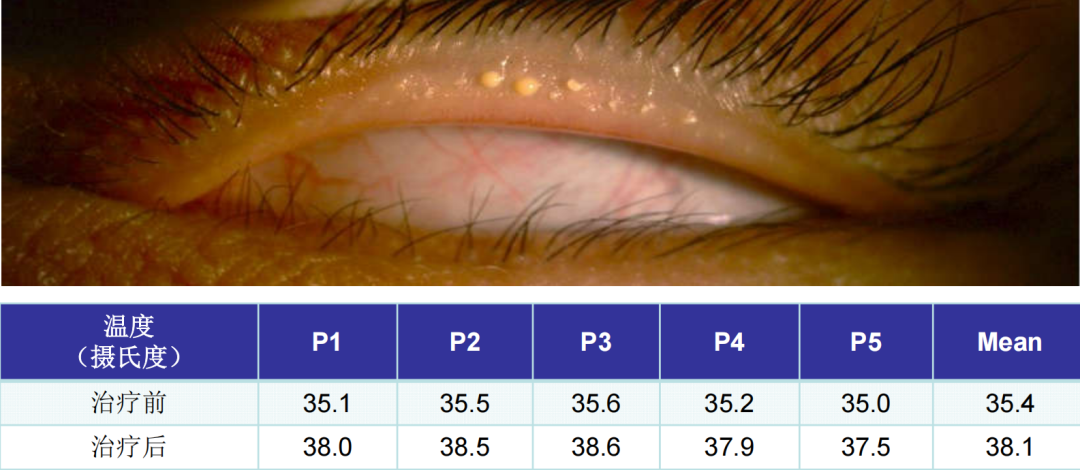
3、 Reduce the growth of bacteria and demodex near the eyelid margin
It has been found that the eradication rate of demodex blepharitis patients after one month of IPL treatment is 55%, while the life cycle of demodex is 15 days. It is speculated that IPL may act on the germ cells of demodex and affect its reproductive capacity.
The bacteria and toxins carried by demodex are important factors to induce the immune response of the body, mainly including some Staphylococcus, Streptococcus and Bacillus.
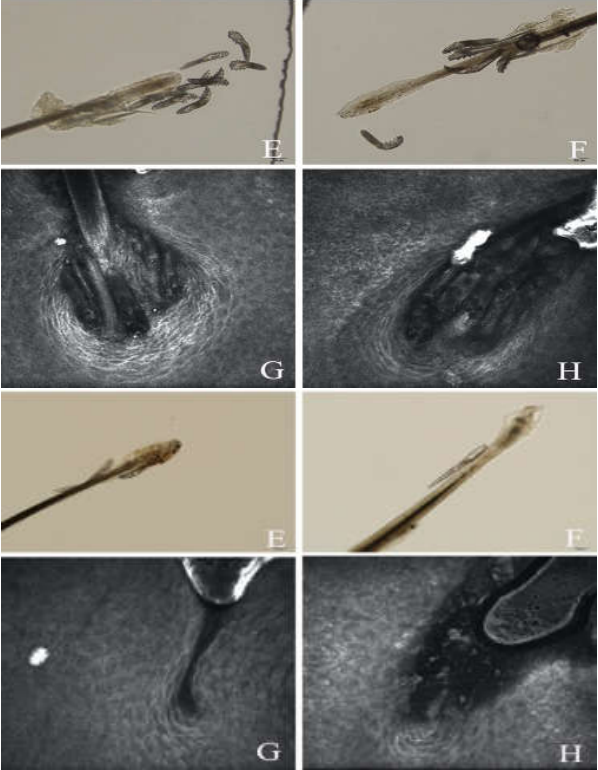
4、 Photobiological regulation
IPL can up regulate the expression of anti-inflammatory factors and inhibit the expression of proinflammatory factors;
Adjust nerve function: improve peripheral nerve function, enhance nerve activity, and relieve ocular surface neurogenic pain;
Promote the regeneration of collagen fibers;
Reduce the renewal of glandular epithelial cells;
It inhibits the production of matrix metalloproteinases (MMP).
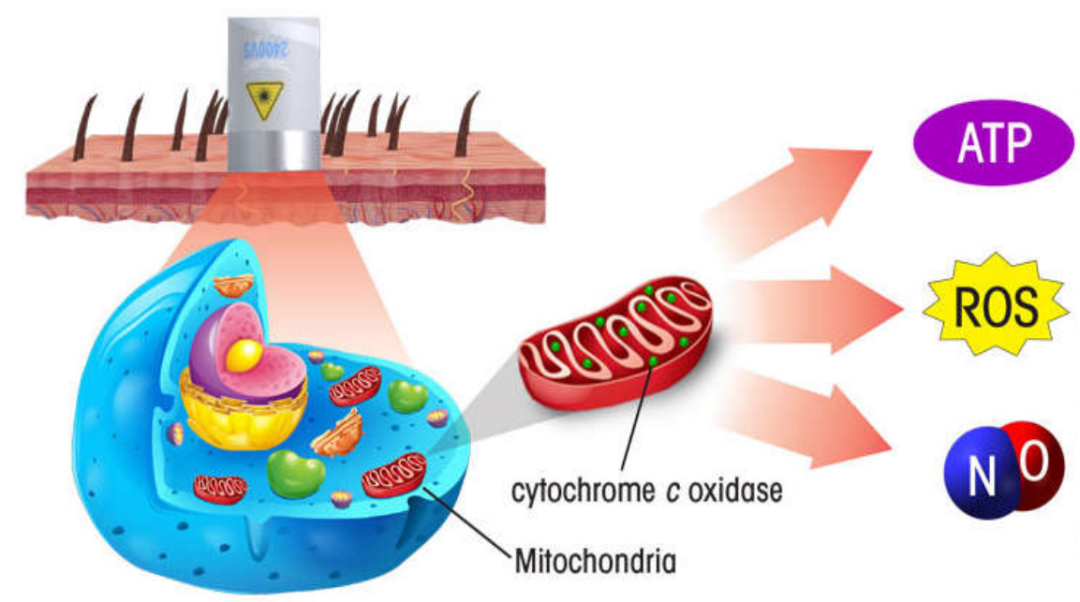

The treatment of ocular surface diseases with intense pulsed light not only has a solid theoretical basis, but also has been supported by many clinical data at home and abroad.

The clinical data summarized by Fan Jingjing (attending physician, graduate of Peking University Medical Department) from the First Affiliated Hospital of Zhengzhou University in China shows that the ophthalmic applicable diseases of intense pulsed light (IPL) treatment are mainly meibomian gland dysfunction (MGD) and related dry eyes, eyelid margin related keratoconjunctival lesions (BKC), wheat granuloma, multiple recurrent chalazion, etc.
1、 IPL treatment of meibomian gland dysfunction (MGD) cases
Wu X, male, 18 years old, student;
The feeling of foreign body in both eyes is dry and astringent for more than 2 months, which is aggravated when looking at mobile phones. She used to use artificial tears such as sodium hyaluronate and polyvinyl alcohol, but the effect was not good. No other systemic diseases or eye surgery history. Physical examination binocular visual acuity: naked eye 1.0;
Anterior segment slit lamp examination: ester tincture obstruction at the opening of meibomian gland, and a small amount of lipid like secretion at the eyelid margin. Eyelashes are fair, conjunctival congestion (-), cornea is clear, and other anterior segments (-);
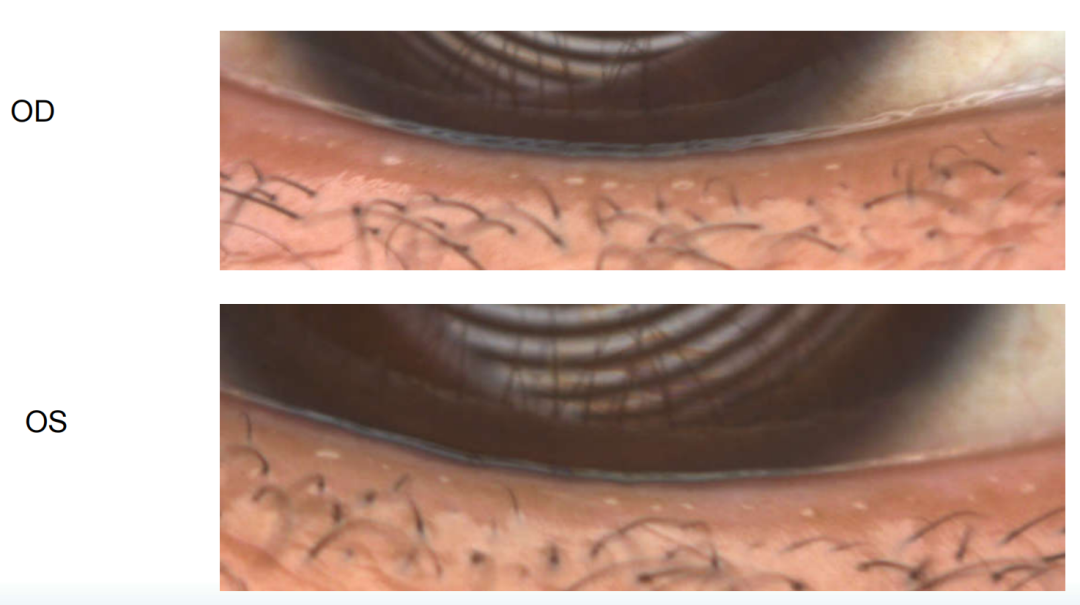
Diagnosis: MGD in both eyes
medication:
Eye drops for removing protein from calf blood, 4 times a day, point at both eyes
Diclofenac sodium eye drops, twice a day, double eye drops
Physical therapy: (do EYESIS intense pulse light+meibomian gland massage) * 2
Comparison of Schirmer test results before treatment (2021.11.16) and after treatment (2021.12.21):
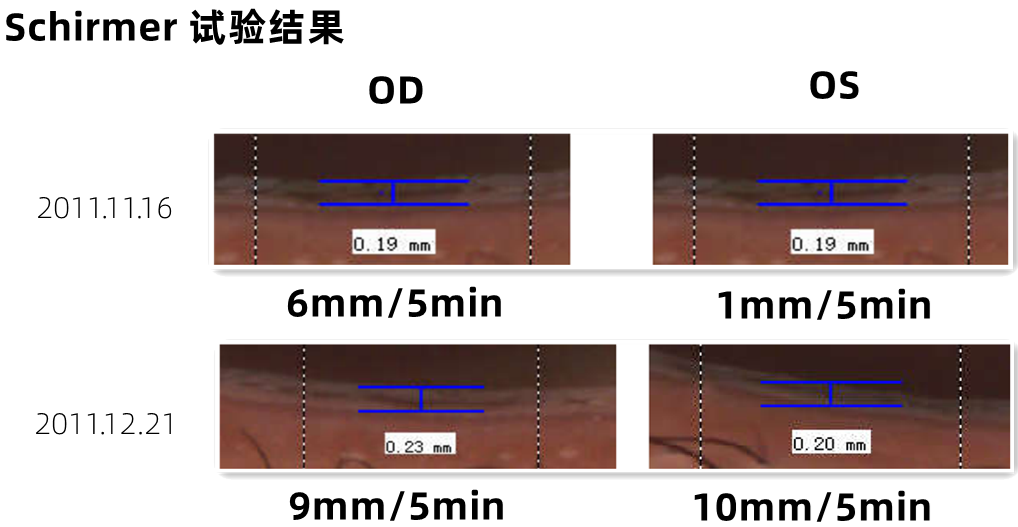
Comparison of dry eye analysis results before and after treatment:
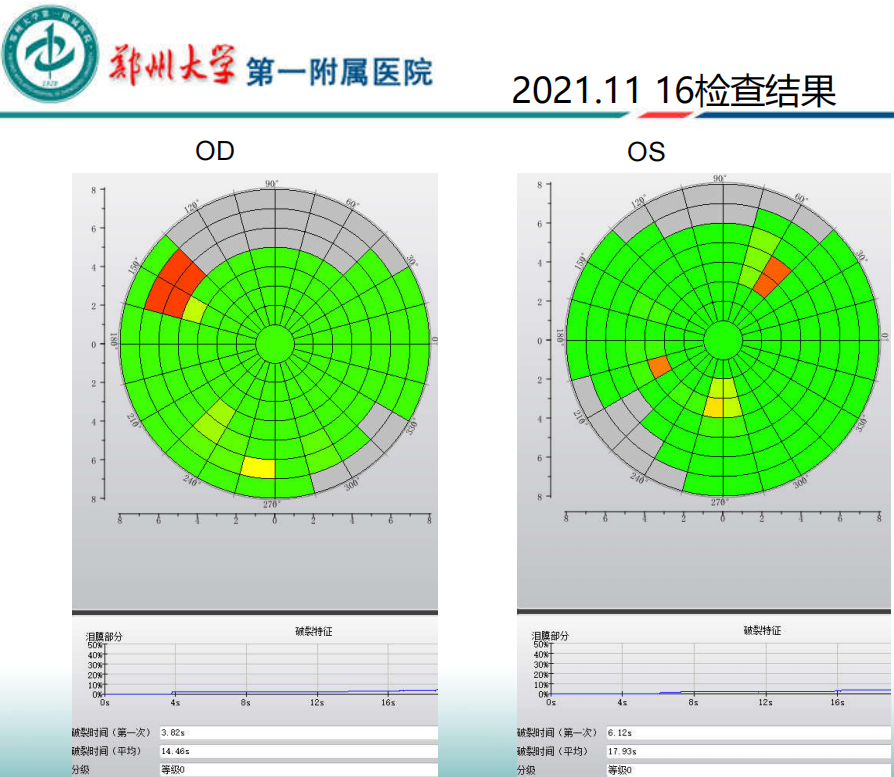
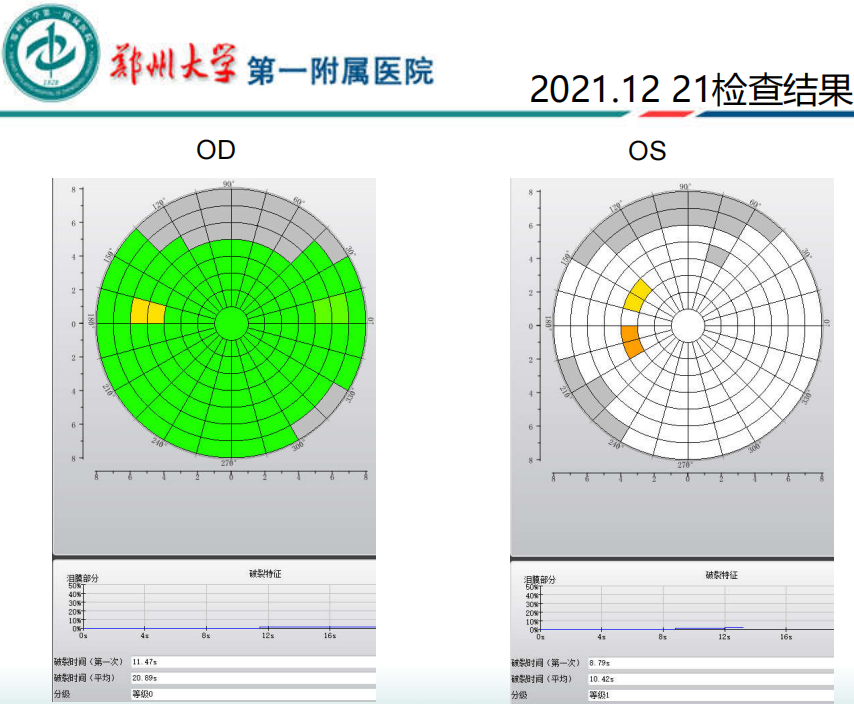
Summary:
It was found that the patients who had undergone 3-6 times of IPL+meibomian gland massage for diagnosis due to dry eyes and MGD,
(1) IPL is effective in improving the symptoms of MGD dry eye patients;
(2) With the progress of IPL treatment, the improvement of the character of eyelid margin opening and meibomian gland secretion can also be seen;
(3) The shape of the palpebral margin is caused by the patient's long-term disease status, so it does not improve significantly during IPL treatment.
2、 Cases of blepharitis associated keratoconjunctival lesions (BKC) treated with IPL
Zhang Xqin, female, 66 years old, went to the doctor for more than one month due to dry, itchy, red eyes and vision loss in both eyes, and the left eye was heavy. He once went to the hospital to diagnose "erosive keratitis of the left eye", and was treated with calf blood, Befloxacin, left oxygen, cyclosporine, erythromycin eye ointment, etc., but no obvious improvement was found.
Check:
Vision: OD 0.6, OS 0.1
NCT:OD 10mmhg、OS 9mmhg
2021.12.21, Results of anterior segment examination before treatment:
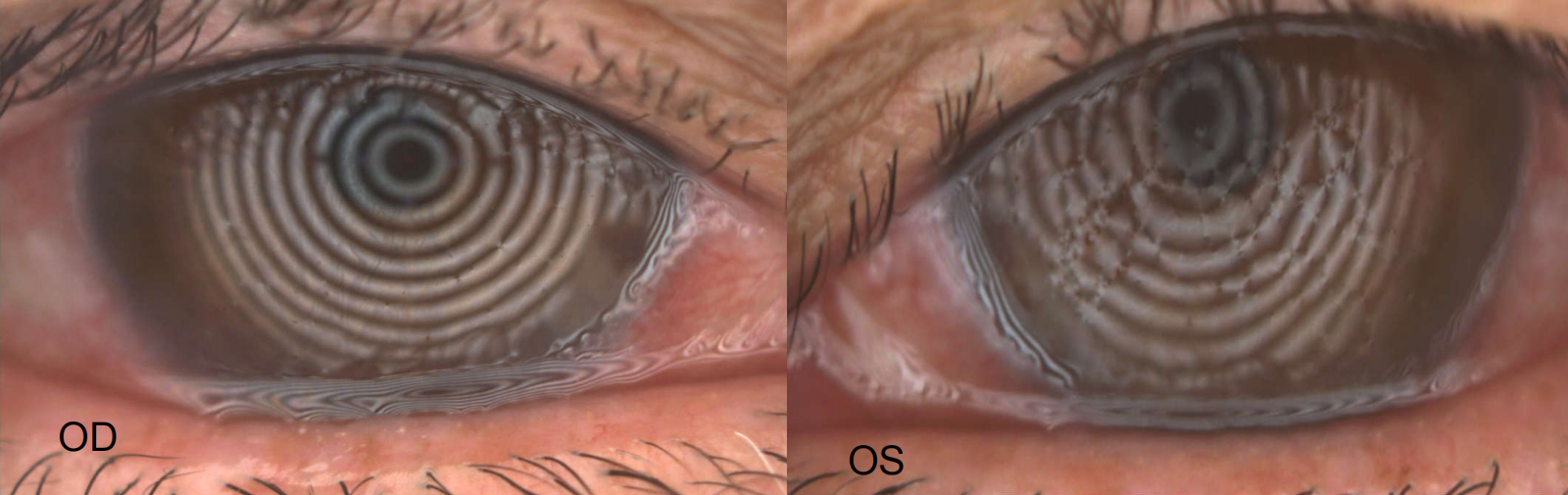
Diagnosis: BKC in both eyes (eyelid margin related keratoconjunctivopathy)
medication:
Calf blood deproteinized eye gel, 3 times a day, point both eyes;
Fluminolone eye drops, 4 times a day, point both eyes;
Dianbishu Eye Cream is applied to the eyelid margin of both eyes twice a day.
Physical therapy: EYESIS intense pulsed light * 3 times for both eyes, and eyelid margin cleaning once every other day.
The patient was hospitalized, during which the patient's condition changed.

2022.1.12, Results of anterior segment examination after treatment:
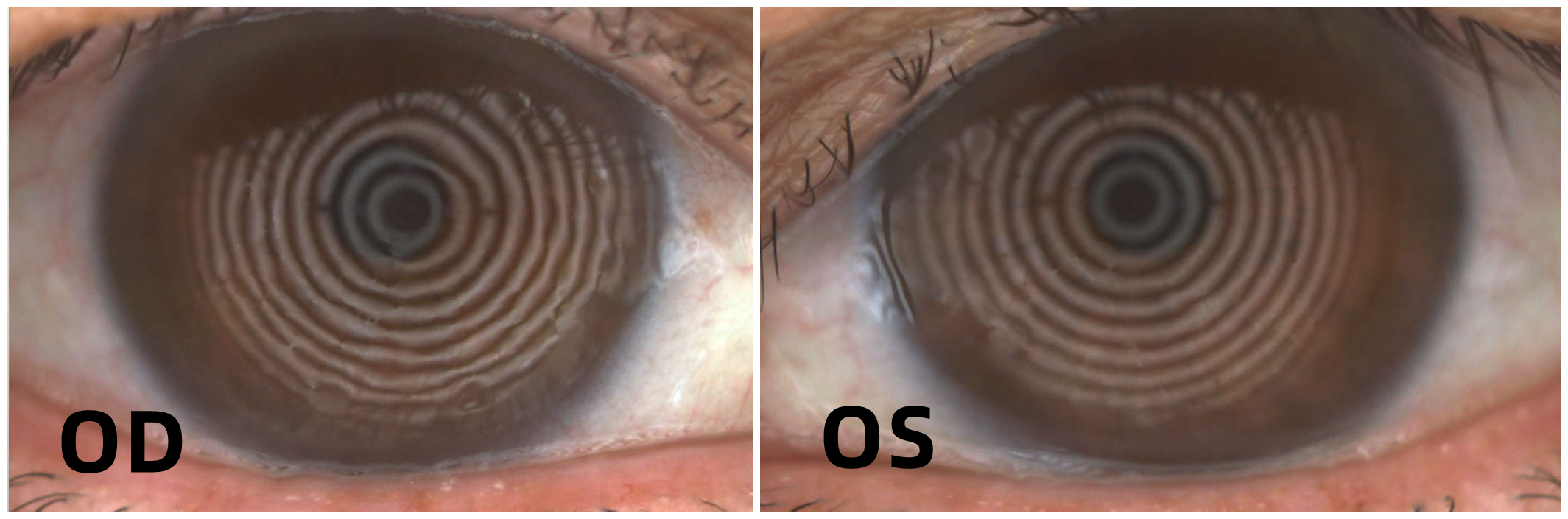
Summary: The key point of treatment for patients with BKC is to make a clear diagnosis. Patients often complain of decreased vision and keratoconjunctival diseases as signs, so they are easy to ignore the problem of eyelid margin and are misdiagnosed as keratoconjunctival diseases. In fact, if this kind of patients can solve the palpebral margin disease, the keratoconjunctival disease will naturally be alleviated.
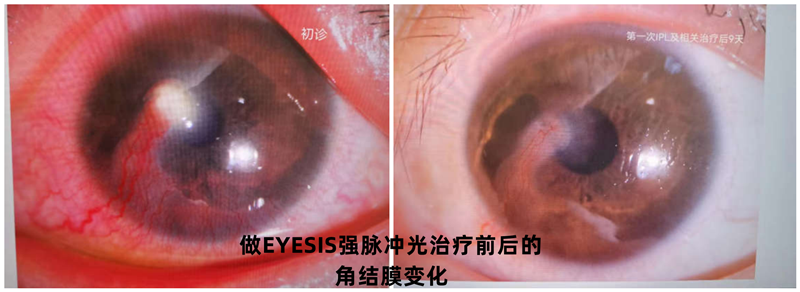
3、 IPL in the Treatment of Cerella and Meibomian Gland Cysts
Wang, female, 27 years old. The lower eyelid of the left eye was red, swollen, hot and painful for one day, and levofloxacin eye drops were applied for one day, but there was no significant improvement.
Diagnosis: acute blepharitis of left eye
Physical therapy plan: The left eye was treated with EYESIS strong pulse light once, and the redness and swelling symptoms disappeared after 1 day of reexamination.

Summary:
1. Most patients with acute blepharitis (in the early stage of redness and swelling, within 1-2 days of onset) can take effect after one IPL treatment, which can be used with local anti-inflammatory drugs.
2. The treatment time of acute blepharitis should be properly selected. IPL treatment after the abscess starts to form will accelerate the course of the disease, promote the rapid formation of the abscess, and give the patient a feeling of aggravation after treatment. Therefore, care should be taken to communicate before treatment.
4、 IPL treatment of children with chalazion
Yuan X yi, female, 3 years old. The lower eyelid of the right eye has been red and swollen for more than 2 months. Antibiotic eye ointment has been applied intermittently to reduce the redness and swelling, but there has been no obvious change in the last 2 weeks. The hard strips can be touched under the corresponding eyelid skin.
Physical therapy plan: The right eye was treated with EYESIS intense pulse light for 4 times.
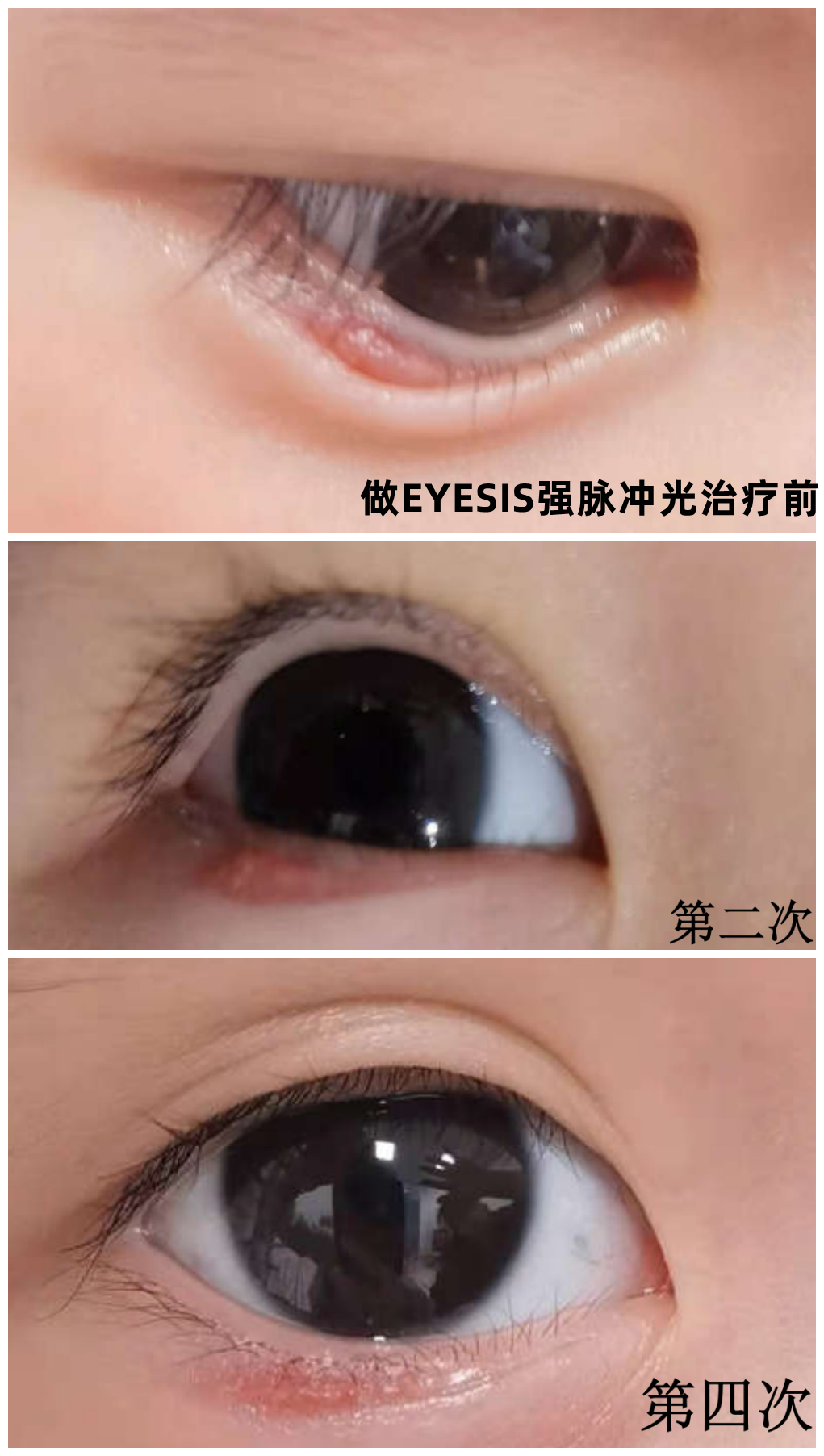
Summary:
1. Intense pulsed light (IPL) is effective in the treatment of children's chalazion.
2. The treatment process of EYESIS is simple and efficient, with high acceptance of children and parents.
3. It usually takes 3-5 times for EYESIS to treat children's chalazion, and the times should be adjusted according to the size of the chalazion and the main involved parts. The effect of IPL on facial chalazion is better.
4. The treatment of upper and lower eyelid chalazion has good effect in IPL, but the treatment of upper eyelid refractory chalazion may not perform well in IPL.
5. No serious adverse reactions were observed in children with IPL, and EYESIS was safe in the treatment of children with chalazion.
Medical workers can not only apply it to today's clear indications, but also use it to explore the treatment of other ocular surface diseases in the future. We believe that the development and promotion of EYESIS special intense pulsed light treatment equipment for ophthalmology will certainly open a new chapter in the treatment of dry eyes and ocular surface diseases.

